Math Is Fun Forum
You are not logged in.
- Topics: Active | Unanswered
- Index
- » Science HQ
- » Arthritis
Pages: 1
#1 Yesterday 17:15:40
- Jai Ganesh
- Administrator

- Registered: 2005-06-28
- Posts: 53,524
Arthritis
Arthritis
Gist
Arthritis is inflammation of one or more joints, causing pain, stiffness, and swelling. Common types include osteoarthritis (wear-and-tear) and rheumatoid arthritis (autoimmune). Key risk factors include age, genetics, and obesity. Treatments include medications, physical therapy, and lifestyle changes, aiming to manage symptoms and improve function.
Good approaches for arthritis include low-impact exercise, weight management, heat/cold therapy, and an anti-inflammatory diet rich in fruits, vegetables, fish, and whole grains, while avoiding processed foods and sugar, alongside potential medications, physical therapy, and sometimes surgery for severe cases, with lifestyle changes being key. Balancing activity and rest, maintaining good posture, and using assistive devices can also significantly ease symptoms.
Summary
Arthritis is a general medical term used to describe a disorder in which the smooth cartilagenous layer that lines a joint is lost, resulting in bone grinding on bone during joint movement. Symptoms generally include joint pain and stiffness. Other symptoms may include redness, warmth, swelling, and decreased range of motion of the affected joints. In certain types of arthritis, other organs, such as the skin, are also affected. Onset can be gradual or sudden.
There are several types of arthritis. The most common forms are osteoarthritis (most commonly seen in weightbearing joints) and rheumatoid arthritis. Osteoarthritis usually occurs as a person ages and often affects the hips, knees, shoulders, and fingers. Rheumatoid arthritis is an autoimmune disorder that often affects the hands and feet. Other types of arthritis include gout, lupus, and septic arthritis. These are inflammatory based types of rheumatic disease.
Early treatment for arthritis commonly includes resting the affected joint and conservative measures such as heating or icing. Weight loss and exercise may also be useful to reduce the force across a weightbearing joint. Medication intervention for symptoms depends on the form of arthritis. These may include anti-inflammatory medications such as ibuprofen and paracetamol (acetaminophen). With severe cases of arthritis, joint replacement surgery may be necessary.
Osteoarthritis is the most common form of arthritis affecting more than 3.8% of people, while rheumatoid arthritis is the second most common affecting about 0.24% of people. In Australia about 15% of people are affected by arthritis, while in the United States more than 20% have a type of arthritis. Overall arthritis becomes more common with age. Arthritis is a common reason people are unable to carry out their work and can result in decreased ability to complete activities of daily living. The term arthritis is derived from arthr- (meaning 'joint') and -itis (meaning 'inflammation').
Details:
Overview
Arthritis and other rheumatic diseases are common conditions that cause pain, swelling, and limited movement. They affect joints and connective tissues around the body. Millions of people in the U.S. have some form of arthritis.
Arthritis means redness and swelling (inflammation) of a joint. A joint is where 2 or more bones meet. There are more than 100 different arthritis diseases. Rheumatic diseases include any condition that causes pain, stiffness, and swelling in joints, muscles, tendons, ligaments, or bones. Arthritis is usually ongoing (chronic).
Arthritis and other rheumatic diseases are more common in women than men. These conditions are often found in older people. But people of all ages may be affected.
The 2 most common forms of arthritis are:
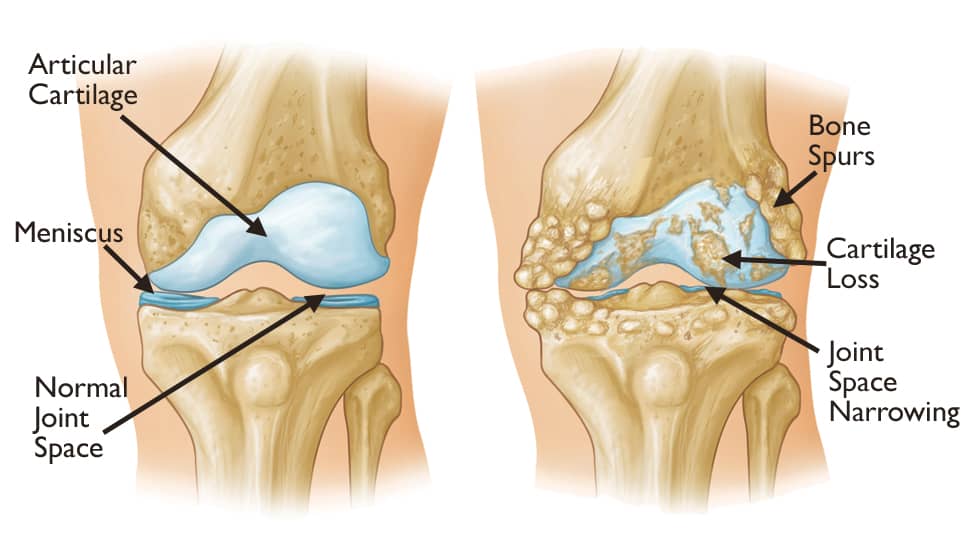
* Osteoarthritis. This is the most common type of arthritis. It is a chronic disease of the joints, especially the weight-bearing joints of the knee, hip, and spine. It destroys the padding on the ends of bones (cartilage) and narrows the joint space. It can also cause bone overgrowth, bone spurs, and reduced function. It occurs in most people as they age. It may also occur in young people from an injury or overuse.
* Rheumatoid arthritis. This is an autoimmune disease that causes inflammation in the joint linings. The inflammation may affect all the joints. It can also affect organs, such as the heart or lungs.
Other forms of arthritis or related disorders include:
* Gout. This condition causes uric acid crystals to build up in small joints, such as the big toe. It causes pain and inflammation.
* Lupus. This is a chronic autoimmune disorder. It causes periods of inflammation and damage in joints, tendons, and organs.
* Scleroderma. This autoimmune disease causes thickening and hardening of the skin and other connective tissue in the body.
* Ankylosing spondylitis. This form of arthritis causes inflammation of the spinal joints. It may lead to severe chronic pain and discomfort. In more advanced cases, sections of the bones fuse together in an immobile position. It can also cause inflammation in other parts of the body. Though it primarily affects the spine, it can also affect the shoulders, hips, ribs, and the small joints of the hands and feet.
* Juvenile idiopathic arthritis or juvenile rheumatoid arthritis. This is a form of arthritis in children under the age of 16 that causes inflammation and joint stiffness. Children may have symptoms that last a limited time, such as a few months or years or in some cases a lifetime. Getting diagnosed and treated early may help prevent joint damage.
What causes arthritis?
The cause depends on the type of arthritis. Osteoarthritis is caused by wear and tear of the joint over time or because of overuse. Rheumatoid arthritis, lupus, and scleroderma are caused by the body’s immune system attacking the body’s own tissues. Gout is caused by the buildup of crystals in the joints. Some forms of arthritis can be linked to genes. People with genetic marker HLA-B27 have a higher risk for ankylosing spondylitis. For some other forms of arthritis, the cause is not known.
Who is at risk for arthritis?
Some risk factors for arthritis that can’t be changed include:
* Age. The older you are, the more likely you are to have arthritis.
* Gender. Women are more likely to have arthritis than men.
* Heredity. Some types of arthritis are linked to certain genes.
Risk factors that may be changed include:
* Weight. Being overweight or obese can damage your knee joints. This can make them more likely to develop osteoarthritis.
* Injury. A joint that has been damaged by an injury is more likely to develop arthritis at some point.
* Infection. Reactive arthritis can affect joints after an infection.
* Your job. Work that involves repeated bending or squatting can lead to knee arthritis.
What are the symptoms of arthritis?
Each person’s symptoms may vary. The most common symptoms include:
* Pain in 1 or more joints that doesn’t go away, or comes back.
* Warmth and redness in 1 or more joints.
* Swelling in 1 or more joints.
* Stiffness in 1 or more joints.
* Trouble moving 1 or more joints in a normal way.
These symptoms can look like other health conditions. Always see your health care provider for a diagnosis.
How is arthritis diagnosed?
Your provider will take your medical history and give you a physical exam. Tests may also be done. These include blood tests, such as:
* Antinuclear antibody test. This checks antibody levels in the blood.
* Complete blood count. This checks if your white blood cell, red blood cell, and platelet levels are normal.
* Creatinine. This test checks for kidney disease.
* Sedimentation rate. This test can find inflammation.
* Hematocrit. This test measures the number of red blood cells.
* RF (rheumatoid factor) and CCP (cyclic citrullinated peptide) antibody tests. These can help diagnose rheumatoid arthritis.
* White blood cell count. This checks the level of white blood cells in your blood.
* Uric acid. This helps diagnose gout.
Other tests may be done, such as:
* Joint aspiration (arthrocentesis). A small sample of synovial fluid is taken from a joint. It's tested to see if crystals or bacteria are present.
* X-rays or other imaging tests. These can tell how damaged a joint is.
* Urine test. This checks for protein and different kinds of blood cells.
* HLA tissue typing. This looks for genetic markers of ankylosing spondylitis.
* Skin biopsy. Tiny tissue samples are removed and checked under a microscope. This test helps to diagnose a type of arthritis that involves the skin, such as lupus or psoriatic arthritis.
* Muscle biopsy. Tiny tissue samples are removed and checked under a microscope. This test helps to diagnose conditions that affect muscles.
How is arthritis treated?
Treatment will depend on your symptoms, your age, and your general health. It will also depend on what type of arthritis you have and how bad the condition is. A treatment plan is tailored to each person with their provider.
There is no known cure for arthritis. The goal of treatment is often to limit pain and inflammation and to help the joint work. Treatment plans often use both short-term and long-term methods.
Short-term treatments include:
* Medicines. Short-term relief for pain and inflammation may include pain relievers, such as acetaminophen, aspirin, ibuprofen, or other nonsteroidal anti-inflammatory medicines.
* Heat and cold. Pain may be eased by using moist heat (warm bath or shower) or dry heat (heating pad) on the joint. Pain and swelling may be eased with cold (ice pack wrapped in a thin towel) on the joint.
* Joint immobilization. Using a splint or brace can help a joint rest and protect it from more injury.
* Massage. Lightly massaging painful muscles may increase blood flow and bring warmth to the muscle.
* Transcutaneous electrical nerve stimulation (TENS). Pain may be eased with a TENS device. The device sends mild, electrical pulses to nerve endings in the painful area. This blocks pain signals to the brain and changes how you feel pain.
* Acupuncture. Thin needles are inserted at certain points in the body. It may help the release of natural pain-relieving chemicals made by the nervous system. The procedure is done by a licensed provider.
Long-term treatments include:
* Disease-modifying antirheumatic drugs. These prescription medicines may slow down the disease and treat any immune system problems linked to the disease. Examples of these medicines include methotrexate, hydroxychloroquine, sulfasalazine, and chlorambucil.
* Corticosteroids. Corticosteroids reduce inflammation and swelling. These medicines, such as prednisone, can be taken by mouth (orally) or as a shot.
* Hyaluronic acid therapy. This is a joint fluid that appears to break down in people with osteoarthritis. It can be injected into a joint, such as the knee to help ease symptoms.
* Surgery. There are many types of surgery, depending on which joints are affected. Surgery may include arthroscopy, fusion, or joint replacement. Full recovery after surgery may take up to 6 months. A rehabilitation program after surgery is an important part of the treatment.
Arthritis treatment can include a team of health care providers, such as:
* Orthopedist or orthopedic surgeon.
* Rheumatologist.
* Physiatrist.
* Primary care (family medicine or internal medicine).
* Rehabilitation nurse.
* Dietitian.
* Physical therapist.
* Occupational therapist.
* Social worker.
* Psychologist or psychiatrist.
* Recreational therapist.
* Vocational therapist.
What are possible complications of arthritis?
Because arthritis causes joints to get worse over time, it can cause disability. It can cause pain and movement problems. You may be less able to carry out normal daily activities and tasks.
Living with arthritis
There is no known cure for arthritis. But it’s important to help keep joints working by reducing pain and inflammation. Work on a treatment plan with your provider that includes medicine and therapy. Work on lifestyle changes that can improve your quality of life. Lifestyle changes include:
* Weight loss. Extra weight puts more stress on weight-bearing joints, such as the hips and knees.
* Exercise. Some exercises may help reduce joint pain and stiffness. These include swimming, walking, low-impact aerobic exercise, and range-of-motion exercises. Stretching exercises may also help keep the joints flexible.
* Activity and rest. To reduce stress on your joints, switch between activity and rest. This can help protect your joints and reduce your symptoms.
* Using assistive devices. Canes, crutches, and walkers can help keep stress off certain joints and improve balance. Make sure walkers, canes, and other mobility devices are adjusted to meet your height and posture.
* Using adaptive equipment. Resachers and grabbers let you extend your reach and reduce straining. Dressing aids help you get dressed more easily.
* Managing use of medicines. Long-term use of some anti-inflammatory medicines can lead to stomach bleeding and other possible side effects. Work with your to create a plan to reduce this risk and manage your pain.
When to contact your doctor
Contact your if you have questions about your medicines, your symptoms get worse, or you have new symptoms.
Additional Information
Arthritis is extremely common, especially in people older than 50. It causes joint pain, stiffness and inflammation. Your provider will help you understand which type of arthritis you have, what’s causing it and which treatments you’ll need. You may need a joint replacement if you have severe arthritis that you can’t manage with other treatments.
Overview:
What is arthritis?
Arthritis is a disease that causes damage in your joints. Joints are places in your body where two bones meet.
Some joints naturally wear down as you age. Lots of people develop arthritis after that normal, lifelong wear and tear. Some types of arthritis happen after injuries that damage a joint. Certain health conditions also cause arthritis.
Arthritis can affect any joint, but is most common in people’s:
* Hands and wrists.
* Knees.
* Hips.
* Feet and ankles.
* Shoulders.
* Lower back (lumbar spine).
A healthcare provider will help you find ways to manage symptoms like pain and stiffness. Some people with severe arthritis eventually need surgery to replace their affected joints.
Visit a healthcare provider if you’re experiencing joint pain that’s severe enough to affect your daily routine or if it feels like you can’t move or use your joints as well as usual.
Types of arthritis
There are more than 100 different types of arthritis. Some of the most common types include:
* Osteoarthritis: Wear and tear arthritis.
* Rheumatoid arthritis: Arthritis that happens when your immune system mistakenly damages your joints.
* Gout: Arthritis that causes sharp uric acid crystals to form in your joints.
* Ankylosing spondylitis: Arthritis that affects joints near your lower back.
* Psoriatic arthritis: Arthritis that affects people who have psoriasis.
* Juvenile arthritis: Arthritis in kids and teens younger than 16.
Depending on which type of arthritis you have, it can break down the natural tissue in your joint (degeneration) or cause inflammation (swelling). Some types cause inflammation that leads to degeneration.
How common is arthritis?
Arthritis is extremely common. Experts estimate that more than one-third of Americans have some degree of arthritis in their joints.
Osteoarthritis is the most common type. Studies have found that around half of all adults will develop osteoarthritis at some point.
Symptoms and Causes
There are more than 100 types of arthritis, but they share several common signs and symptoms.
The most common signs and symptoms of arthritis usually affect your joints and your ability to use them.
What are arthritis symptoms and signs?
The most common arthritis symptoms and signs include:
* Joint pain.
* Stiffness or reduced range of motion (how far you can move a joint).
* Swelling (inflammation).
* Skin discoloration.
* Tenderness or sensitivity to touch around a joint.
* A feeling of heat or warmth near your joints.
Where you experience symptoms depends on which type of arthritis you have, and which of your joints it affects.
Some types of arthritis cause symptoms in waves that come and go called flares or flare-ups. Others make your joints feel painful or stiff all the time, or after being physically active.
What is the main cause of arthritis?
What causes arthritis varies depending on which type you have:
* Osteoarthritis happens naturally as you age — a lifetime of using your joints can eventually wear down their cartilage cushioning.
* You may develop gout if you have too much uric acid in your blood (hyperuricemia).
* Your immune system can cause arthritis (including rheumatoid arthritis) when it damages your joints by mistake.
* Certain viral infections (including COVID-19) can trigger viral arthritis.
* Sometimes, arthritis happens with no cause or trigger. Providers call this idiopathic arthritis.
What are the risk factors?
Anyone can develop arthritis, but some factors may make you more likely to, including:
* Tobacco use: Smoking and using other tobacco products increases your risk.
* Family history: People whose biological family members have arthritis are more likely to develop it.
* Activity level: You might be more likely to have arthritis if you aren’t physically active regularly.
* Other health conditions: Having autoimmune diseases, obesity or any condition that affects your joints increases the chances you’ll develop arthritis.
Some people have a higher arthritis risk, including:
* People older than 50.
* Females.
* Athletes, especially those who play contact sports.
* People who have physically demanding jobs or do work that puts a lot of stress on their joints (standing, crouching, being on your hands and knees for a long time, etc.).
At what age does arthritis usually start?
Arthritis can develop at any age. When it starts depends on which type you have and what’s causing it.
In general, osteoarthritis affects adults older than 50. Rheumatoid arthritis usually develops in adults age 30 to 60.
Other types that have a more direct cause usually start closer to that specific trigger. For example, people with post-traumatic arthritis don’t develop it until after their joints are injured, and gout doesn’t develop until after you’ve had high uric acid levels for at least several months.
Talk to a healthcare provider about your unique arthritis risk, and when you should start watching for signs or changes in your joints.
Diagnosis and Tests:
How do healthcare providers diagnose arthritis?
A healthcare provider will diagnose arthritis with a physical exam. They’ll examine your affected joints and ask about your symptoms. Tell your provider when you first noticed symptoms like pain and stiffness, and if any activities or times of day make them worse.
Your provider will probably check your range of motion (how far you can move a joint). They may compare one joint’s range of motion to other, similar joints (your other knee, ankle or fingers, for example).
Arthritis tests
Your provider might use imaging tests to take pictures of your joints, including:
* X-ray.
* Ultrasound.
* Magnetic resonance imaging (MRI).
* A computed tomography (CT) scan.
These tests can help your provider see damage inside your joints. They can also help your provider rule out other injuries or issues that might cause similar symptoms, like bone fractures (broken bones).
Your provider may use blood tests to check your uric acid levels if they think you have gout. Blood tests can also show signs of infections or autoimmune diseases.
Management and Treatment:
What is arthritis treatment?
There’s no cure for arthritis, but your healthcare provider will help you find treatments that manage your symptoms. Which treatments you’ll need depend on what’s causing the arthritis, which type you have and which joints it affects.
The most common arthritis treatments include:
* Over-the-counter (OTC) anti-inflammatory medicine like NSAIDs or acetaminophen.
* Corticosteroids (prescription anti-inflammatory medicine, including cortisone shots).
* Disease-modifying antirheumatic drugs (DMARDs) if you have rheumatoid or psoriatic arthritis.
* Physical therapy or occupational therapy can help you improve your strength, range of motion and confidence while you’re moving.
* Surgery (usually only if nonsurgical treatments don’t relieve your symptoms).
Arthritis surgery
You may need surgery if you have severe arthritis and other treatments don’t work. The two most common types of arthritis surgery are joint fusion and joint replacement.
Joint fusion is exactly what it sounds like: surgically joining bones together. It’s most common for bones in your spine (spinal fusion) or your ankle (ankle fusion).
If your joints are damaged or you’ve experienced bone loss, you might need an arthroplasty (joint replacement). Your surgeon will remove your damaged natural joint and replace it with a prosthesis (artificial joint). You might need a partial or total joint replacement.
Your provider or surgeon will tell you which type of surgery you’ll need and what to expect.
Outlook / Prognosis:
What can I expect if I have arthritis?
You should expect to manage arthritis symptoms for a long time (probably the rest of your life). Your provider will help you find treatments that reduce how much (and how often) arthritis impacts your daily routine.
Some people with arthritis experience more severe symptoms as they age. Ask your provider how often you should have follow-up visits to check for changes in your joints.
It appears to me that if one wants to make progress in mathematics, one should study the masters and not the pupils. - Niels Henrik Abel.
Nothing is better than reading and gaining more and more knowledge - Stephen William Hawking.
Offline
Pages: 1
- Index
- » Science HQ
- » Arthritis