Math Is Fun Forum
You are not logged in.
- Topics: Active | Unanswered
Pages: 1
#1 2026-03-30 20:47:18
- Jai Ganesh
- Administrator

- Registered: 2005-06-28
- Posts: 53,813
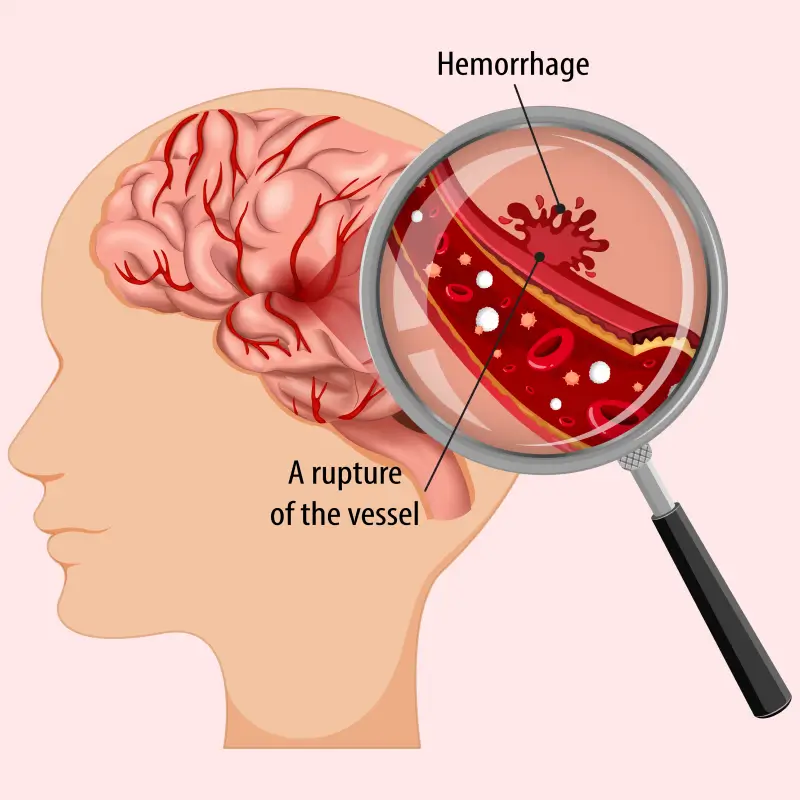
Cerebral Hemorrhage
Cerebral Hemorrhage
Gist
A cerebral hemorrhage (brain bleed) is a life-threatening type of stroke occurring when an artery in the brain bursts or blood leaks into brain tissue, causing high pressure and oxygen deprivation. Common symptoms include sudden, severe headaches, numbness, weakness, confusion, and vomiting. Treatment includes urgent blood pressure control, medication for seizures, or surgery to relieve intracranial pressure.
What is the main cause of cerebral hemorrhage?
The most common causes of a brain hemorrhage are: Head trauma - Injuries to the head are the most common reason for a brain hemorrhage to occur in people younger than 50 years old. High blood pressure - High blood pressure, if left untreated, can weaken the blood vessel walls and lead to a brain hemorrhage.
Summary
Intracerebral hemorrhage (ICH) is a devastating form of stroke with high morbidity and mortality. This review article focuses on the epidemiology, cause, mechanisms of injury, current treatment strategies, and future research directions of ICH. Incidence of hemorrhagic stroke has increased worldwide over the past 40 years, with shifts in the cause over time as hypertension management has improved and anticoagulant use has increased. Preclinical and clinical trials have elucidated the underlying ICH cause and mechanisms of injury from ICH including the complex interaction between edema, inflammation, iron-induced injury, and oxidative stress. Several trials have investigated optimal medical and surgical management of ICH without clear improvement in survival and functional outcomes. Ongoing research into novel approaches for ICH management provide hope for reducing the devastating effect of this disease in the future. Areas of promise in ICH therapy include prognostic biomarkers and primary prevention based on disease pathobiology, ultra-early hemostatic therapy, minimally invasive surgery, and perihematomal protection against inflammatory brain injury.
Intracerebral hemorrhage (ICH) is a devastating form of stroke characterized by bleeding into the brain parenchyma. Although this form of stroke accounts for only 10% of all strokes in the United States and 6.5% to 19.6% worldwide, mortality from ICH remains as high as 50% at 30 days. Over the past decade, there have been significant advances in the understanding of ICH risk, potential treatments, and outcomes.
Intracerebral hemorrhage (ICH) is a devastating form of stroke characterized by bleeding into the brain parenchyma. Although this form of stroke accounts for only 10% of all strokes in the United States and 6.5% to 19.6% worldwide, mortality from ICH remains as high as 50% at 30 days. Over the past decade, there have been significant advances in the understanding of ICH risk, potential treatments, and outcomes.
Details
Intracerebral hemorrhage (ICH), also known as hemorrhagic stroke, is a sudden bleeding into the tissues of the brain (i.e. the parenchyma), into its ventricles, or into both. An ICH is a type of bleeding within the skull and one kind of stroke (ischemic stroke being the other). Symptoms can vary dramatically depending on the severity (how much blood), acuity (over what timeframe), and location (anatomically) but can include headache, one-sided weakness, numbness, tingling, or paralysis, speech problems, vision or hearing problems, memory loss, attention problems, coordination problems, balance problems, dizziness or lightheadedness or vertigo, nausea/vomiting, seizures, decreased level of consciousness or total loss of consciousness, neck stiffness, and fever.
Hemorrhagic stroke may occur on the background of alterations to the blood vessels in the brain, such as cerebral arteriolosclerosis, cerebral amyloid angiopathy, cerebral arteriovenous malformation, brain trauma, brain tumors and an intracranial aneurysm, which can cause intraparenchymal or subarachnoid hemorrhage.
The biggest risk factors for spontaneous bleeding are high blood pressure and amyloidosis. Other risk factors include alcoholism, low cholesterol, blood thinners, and cocaine use. Diagnosis is typically by CT scan.
Treatment should typically be carried out in an intensive care unit due to strict blood pressure goals and frequent use of both pressors and antihypertensive agents. Anticoagulation should be reversed if possible and blood sugar kept in the normal range. A procedure to place an external ventricular drain may be used to treat hydrocephalus or increased intracranial pressure, however, the use of corticosteroids is frequently avoided. Sometimes surgery to directly remove the blood can be therapeutic.
Cerebral bleeding affects about 2.5 per 10,000 people each year. It occurs more often in males and older people. About 44% of those affected die within a month. A good outcome occurs in about 20% of those affected. Intracerebral hemorrhage, a type of hemorrhagic stroke, was first distinguished from ischemic strokes due to insufficient blood flow, so called "leaks and plugs", in 1823.
Additional Information
A brain bleed (intracranial hemorrhage) is a type of stroke. It causes blood to pool between your brain and skull. It prevents oxygen from reaching your brain. It’s life-threatening and requires quick treatment for the best outcome.
Overview:
What is a brain bleed?
A brain bleed (intracranial hemorrhage) is a type of stroke that causes bleeding in your head.
As your brain can’t store oxygen, it relies on a series of blood vessels to supply its oxygen and nutrients. When a brain bleed occurs, a blood vessel leaks blood or bursts. Blood collects or pools within your skull and brain. This causes pressure against your brain, which prevents oxygen and nutrients from reaching your brain tissues and cells.
Brain bleeds are common after falls or traumatic injuries. They’re also common in people with unmanaged high blood pressure.
A brain bleed is a life-threatening medical emergency. It only takes three to four minutes for your brain cells to die if they don’t receive enough oxygen. Treating a brain bleed quickly leads to the best outcome.
What are the types of brain bleeds?
There are many parts to your brain, so the term “brain bleed” (intracranial hemorrhage) is very broad to healthcare providers. Types of brain bleeds help your healthcare provider identify specifically where the bleeding occurs.
There are two main areas of bleeding:
* Within your skull but outside of brain tissue.
* Inside brain tissue.
To better understand where each type of brain bleed occurs, it helps to know the components within your skull. The brain has three membrane layers (meninges) between the bony skull and brain tissue. The three membranes are the dura mater, arachnoid and pia mater. The purpose of the meninges is to cover and protect your brain. Bleeding can occur anywhere between these three membranes.
Types of brain bleeds within your skull but outside of brain tissue include:
* Epidural bleed: This bleed happens between the skull bone and the outermost membrane layer, the dura mater.
* Subdural bleed: This bleed happens between the dura mater and the arachnoid membrane.
* Subarachnoid bleed: This bleed happens between the arachnoid membrane and the pia mater.
There are two types of brain bleeds that occur inside the brain tissue itself:
* Intracerebral hemorrhage: This bleeding occurs in the lobes, brainstem and cerebellum of your brain. This is bleeding anywhere within the brain tissue itself.
* Intraventricular hemorrhage: This bleeding occurs in your brain’s ventricles, which are specific areas of the brain (cavities) where your body makes cerebrospinal fluid (fluid that protects your brain and spinal cord).
Are brain bleeds fatal?
Brain bleeds can be life-threatening and cause permanent brain damage. The severity and outcome of a brain bleed depend on its cause, location inside of your skull, size of the bleed, the amount of time that passes between the bleed and treatment. Once brain cells die, they don’t come back. Damage can be severe and result in physical, mental and task-based disability.
How common is a brain bleed?
Brain bleeds are a type of stroke. More than 795,000 people in the United States experience a stroke each year.
Symptoms and Causes:
What are the symptoms of a brain bleed?
Symptoms of a brain bleed vary based on the type, but could include:
* Sudden tingling, weakness, numbness or paralysis of your face, arm or leg, particularly on one side of your body.
* Sudden, severe headache.
* Nausea and vomiting.
* Confusion.
* Dizziness.
* Slurred speech.
* Lack of energy, sleepiness.
In addition, you may experience:
* Difficulty swallowing.
* Vision loss.
* Stiff neck.
* Sensitivity to light.
* Loss of balance or coordination.
* Trouble breathing and abnormal heart rate.
* Seizures.
* Loss of consciousness and coma.
What is the first symptom of a brain bleed?
Most people who experience a brain bleed note that the first symptom is a sudden, painful headache.
What causes a brain bleed?
A leaky, broken or burst blood vessel causes a brain bleed. As a result, excess blood pools in your brain. A brain bleed can happen after:
* Head trauma (a fall, car accident, sports injury, etc.).
* A buildup of fatty deposits in your arteries (atherosclerosis).
* A blood clot.
* A weak spot in a blood vessel wall (cerebral aneurysm).
* A leak from abnormally formed connections between arteries and veins (arteriovenous malformation, or AVM).
* A buildup of protein within the artery walls of the brain (cerebral amyloid angiopathy).
* A brain tumor.
What are the risk factors for a brain bleed?
A brain bleed can affect anyone at any age, from newborns to adults. It’s more common among adults over age 65. You may be more at risk of a brain bleed if you experience the following:
* High blood pressure (hypertension).
* Substance use disorder.
* Tobacco use.
* Bleeding conditions or conditions that need treatment with blood thinners (anticoagulants).
* Pregnancy and childbirth-related conditions (eclampsia, postpartum vasculopathy or neonatal intraventricular hemorrhage).
* Conditions that affect how your blood vessel walls form.
What are the complications of a brain bleed?
If not treated quickly, a brain bleed can lead to permanent brain damage or death. A lack of oxygen to your brain can destroy your brain cells and prevent them from communicating with other parts of your body. This affects how your body functions overall, so you may experience:
* Memory loss.
* Difficulty with swallowing, speech and communication.
* Coordination and movement challenges.
* Inability to move part of your body (paralysis).
* Numbness or weakness in part of your body.
* Vision loss.
* Personality changes and/or emotional changes.
Diagnosis and Tests:
How is a brain bleed diagnosed?
A healthcare provider will diagnose a brain bleed after an immediate physical exam, neurological exam and testing. They’ll review your complete medical history and your symptoms first. Then, they’ll order an imaging test like:
* A computed tomography (CT) scan.
* Magnetic resonance imaging (MRI).
* Magnetic resonance angiogram (MRA).
These imaging tests determine the location, extent and, sometimes, the cause of the bleed.
Other tests can help detect a cause and may include:
* Electroencephalogram.
* Chest X-ray.
* Urinalysis.
* Complete blood count (CBC).
* Lumbar puncture (spinal tap).
* Angiography (for an aneurysm or arteriovenous malformation).
It appears to me that if one wants to make progress in mathematics, one should study the masters and not the pupils. - Niels Henrik Abel.
Nothing is better than reading and gaining more and more knowledge - Stephen William Hawking.
Offline
Pages: 1