Math Is Fun Forum
You are not logged in.
- Topics: Active | Unanswered
Pages: 1
#1 2025-02-08 19:06:54
- Jai Ganesh
- Administrator

- Registered: 2005-06-28
- Posts: 53,826
Coagulation
Coagulation
Gist
Blood clotting, or coagulation, is an important process that prevents excessive bleeding when a blood vessel is injured. Platelets (a type of blood cell) and proteins in your plasma (the liquid part of blood) work together to stop the bleeding by forming a clot over the injury.
Coagulation treatment is usually carried out before sedimentation and filtration. During the process, a coagulant is added to water, and its positive charge neutralizes the negative charge of suspended contaminants.
Coagulation consists of three pathways, the extrinsic, intrinsic, and common pathways, that interact together to form a stable blood clot. The extrinsic and intrinsic coagulation pathways both lead into the final common pathway by independently activating factor X.
Summary
Coagulation, in physiology, is the process by which a blood clot is formed. The formation of a clot is often referred to as secondary hemostasis, because it forms the second stage in the process of arresting the loss of blood from a ruptured vessel. The first stage, primary hemostasis, is characterized by blood vessel constriction (vasoconstriction) and platelet aggregation at the site of vessel injury. Under abnormal circumstances, clots can also form in a vessel that has not been breached; such clots can result in the occlusion (blockage) of the vessel.
Clotting is a sequential process that involves the interaction of numerous blood components called coagulation factors. There are 13 principal coagulation factors in all, and each of these has been assigned a Roman numeral, I to XIII. Coagulation can be initiated through the activation of two separate pathways, designated extrinsic and intrinsic. Both pathways result in the production of factor X. The activation of this factor marks the beginning of the so-called common pathway of coagulation, which results in the formation of a clot.
The extrinsic pathway is generally the first pathway activated in the coagulation process and is stimulated in response to a protein called tissue factor, which is expressed by cells that are normally found external to blood vessels. However, when a blood vessel breaks and these cells come into contact with blood, tissue factor activates factor VII, forming factor VIIa, which triggers a cascade of reactions that result in the rapid production of factor X. In contrast, the intrinsic pathway is activated by injury that occurs within a blood vessel. This pathway begins with the activation of factor XII (Hageman factor), which occurs when blood circulates over injured internal surfaces of vessels. Components of the intrinsic pathway also may be activated by the extrinsic pathway; for example, in addition to activating factor X, factor VIIa activates factor IX, a necessary component of the intrinsic pathway. Such cross-activation serves to amplify the coagulation process.
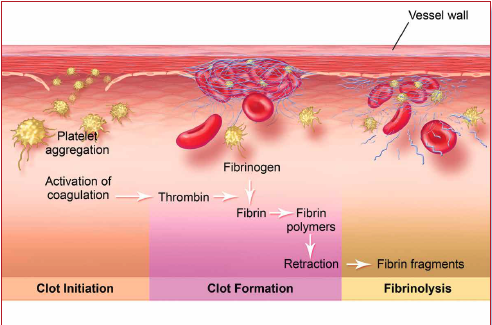
The production of factor X results in the cleavage of prothrombin (factor II) to thrombin (factor IIa). Thrombin, in turn, catalyzes the conversion of fibrinogen (factor I)—a soluble plasma protein—into long, sticky threads of insoluble fibrin (factor Ia). The fibrin threads form a mesh that traps platelets, blood cells, and plasma. Within minutes, the fibrin meshwork begins to contract, squeezing out its fluid contents. This process, called clot retraction, is the final step in coagulation. It yields a resilient, insoluble clot that can withstand the friction of blood flow.
Details
Coagulation, also known as clotting, is the process by which blood changes from a liquid to a gel, forming a blood clot. It results in hemostasis, the cessation of blood loss from a damaged vessel, followed by repair. The process of coagulation involves activation, adhesion and aggregation of platelets, as well as deposition and maturation of fibrin.
Coagulation begins almost instantly after an injury to the endothelium that lines a blood vessel. Exposure of blood to the subendothelial space initiates two processes: changes in platelets, and the exposure of subendothelial platelet tissue factor to coagulation factor VII, which ultimately leads to cross-linked fibrin formation. Platelets immediately form a plug at the site of injury; this is called primary hemostasis. Secondary hemostasis occurs simultaneously: additional coagulation factors beyond factor VII (listed below) respond in a cascade to form fibrin strands, which strengthen the platelet plug.
Coagulation is highly conserved throughout biology. In all mammals, coagulation involves both cellular components (platelets) and proteinaceous components (coagulation or clotting factors). The pathway in humans has been the most extensively researched and is the best understood. Disorders of coagulation can result in problems with hemorrhage, bruising, or thrombosis.
Role in disease
Coagulation defects may cause hemorrhage or thrombosis, and occasionally both, depending on the nature of the defect.
Platelet disorders
Platelet disorders are either congenital or acquired. Examples of congenital platelet disorders are Glanzmann's thrombasthenia, Bernard–Soulier syndrome (abnormal glycoprotein Ib-IX-V complex), gray platelet syndrome (deficient alpha granules), and delta storage pool deficiency (deficient dense granules). Most are rare. They predispose to hemorrhage. Von Willebrand disease is due to deficiency or abnormal function of von Willebrand factor, and leads to a similar bleeding pattern; its milder forms are relatively common.
Decreased platelet numbers (thrombocytopenia) is due to insufficient production (e.g., myelodysplastic syndrome or other bone marrow disorders), destruction by the immune system (immune thrombocytopenic purpura), or consumption (e.g., thrombotic thrombocytopenic purpura, hemolytic-uremic syndrome, paroxysmal nocturnal hemoglobinuria, disseminated intravascular coagulation, heparin-induced thrombocytopenia). An increase in platelet count is called thrombocytosis, which may lead to formation of thromboembolisms; however, thrombocytosis may be associated with increased risk of either thrombosis or hemorrhage in patients with myeloproliferative neoplasm.
Coagulation factor disorders
The best-known coagulation factor disorders are the hemophilias. The three main forms are hemophilia A (factor VIII deficiency), hemophilia B (factor IX deficiency or "Christmas disease") and hemophilia C (factor XI deficiency, mild bleeding tendency).
Von Willebrand disease (which behaves more like a platelet disorder except in severe cases), is the most common hereditary bleeding disorder and is characterized as being inherited autosomal recessive or dominant. In this disease, there is a defect in von Willebrand factor (vWF), which mediates the binding of glycoprotein Ib (GPIb) to collagen. This binding helps mediate the activation of platelets and formation of primary hemostasis.
In acute or chronic liver failure, there is insufficient production of coagulation factors, possibly increasing risk of bleeding during surgery.
Thrombosis is the pathological development of blood clots. These clots may break free and become mobile, forming an embolus or grow to such a size that occludes the vessel in which it developed. An embolism is said to occur when the thrombus (blood clot) becomes a mobile embolus and migrates to another part of the body, interfering with blood circulation and hence impairing organ function downstream of the occlusion. This causes ischemia and often leads to ischemic necrosis of tissue. Most cases of venous thrombosis are due to acquired states (older age, surgery, cancer, immobility). Unprovoked venous thrombosis may be related to inherited thrombophilias (e.g., factor V Leiden, antithrombin deficiency, and various other genetic deficiencies or variants), particularly in younger patients with family history of thrombosis; however, thrombotic events are more likely when acquired risk factors are superimposed on the inherited state.
Pharmacology:
Procoagulants
The use of adsorbent chemicals, such as zeolites, and other hemostatic agents are also used for sealing severe injuries quickly (such as in traumatic bleeding secondary to gunshot wounds). Thrombin and fibrin glue are used surgically to treat bleeding and to thrombose aneurysms. Hemostatic Powder Spray TC-325 is used to treated gastrointestinal bleeding.
Desmopressin is used to improve platelet function by activating arginine vasopressin receptor 1A.
Coagulation factor concentrates are used to treat hemophilia, to reverse the effects of anticoagulants, and to treat bleeding in people with impaired coagulation factor synthesis or increased consumption. Prothrombin complex concentrate, cryoprecipitate and fresh frozen plasma are commonly used coagulation factor products. Recombinant activated human factor VII is sometimes used in the treatment of major bleeding.
Tranexamic acid and aminocaproic acid inhibit fibrinolysis and lead to a de facto reduced bleeding rate. Before its withdrawal, aprotinin was used in some forms of major surgery to decrease bleeding risk and the need for blood products.
Rivaroxaban drug bound to the coagulation factor Xa. The drug prevents this protein from activating the coagulation pathway by inhibiting its enzymatic activity.
Anticoagulants
Anticoagulants and anti-platelet agents (together "antithrombotics") are amongst the most commonly used medications. Anti-platelet agents include aspirin, dipyridamole, ticlopidine, clopidogrel, ticagrelor and prasugrel; the parenteral glycoprotein IIb/IIIa inhibitors are used during angioplasty. Of the anticoagulants, warfarin (and related coumarins) and heparin are the most commonly used. Warfarin affects the vitamin K-dependent clotting factors (II, VII, IX, X) and protein C and protein S, whereas heparin and related compounds increase the action of antithrombin on thrombin and factor Xa. A newer class of drugs, the direct thrombin inhibitors, is under development; some members are already in clinical use (such as lepirudin, argatroban, bivalirudin and dabigatran). Also in clinical use are other small molecular compounds that interfere directly with the enzymatic action of particular coagulation factors (the directly acting oral anticoagulants: dabigatran, rivaroxaban, apixaban, and edoxaban).
It appears to me that if one wants to make progress in mathematics, one should study the masters and not the pupils. - Niels Henrik Abel.
Nothing is better than reading and gaining more and more knowledge - Stephen William Hawking.
Offline
Pages: 1